This article was published in Scientific American’s former blog network and reflects the views of the author, not necessarily those of Scientific American
Here’s a thing I never thought I’d write about. According to research published this summer, if you measure the time it takes for stuff to make its way through your colon, you learn all sorts of things about your health, your microbes, and (this is just a supposition on my part) the nature of your typical conversations at dinner parties. There’s no judgement here - I’m constantly talking about stool at dinner parties.
A lot of times in medicine, there are things we want to know that are tough to measure, and there are things that are easy to measure that are sort of related to things that we want to know. One example is colonic transit time, for which a decent proxy is stool firmness. One of the main jobs of the colon is to reabsorb water from your digestive process, the longer a bolus of waste hangs out, the firmer it gets. Taking a more direct measurement is hard (pass on poop puns please) - you have to send something that can be tracked down one end, and then watch it all the way through - more on this later.
Most of the time, proxy measures are good enough, so the time and expense of more difficult tests can’t be justified, but every now and again it’s worth double checking assumptions. For example, we know that fecal firmness (also avoid alimentary alliteration) is related to colonic transit time. Recent work also shows that firm stool is associated with increased diversity in the microbes in your gut. Other work, very well supported, suggests that people with a lot of diversity in their guts are more healthy, or at least that unhealthy people tend to have less diversity in their gut.
On supporting science journalism
If you're enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
Based on this evidence, it’s easy to tell a compelling story, and pretty soon you get people saying that we should be giving ourselves constipation to cure cancer or something.
Unfortunately, none of the associations are cut and dry, so it’s great that Henrick Roager and colleagues set out to determine if there’s actually a direct link between colonic transit time and health. As you might expect, the answer is complicated.
Colonic transit time is related to bacterial metabolism and mucosal turnover in the gut
In order to measure colonic transit time, they went the difficult route - subjects ingested pellets of “radio opaque markers,” which are basically just balls of some substance that shows up on an or CT scan. Then they were periodically scanned, and some researcher counted to see how many of the pellets were still in the system at various points.
And then they looked at the microbes.
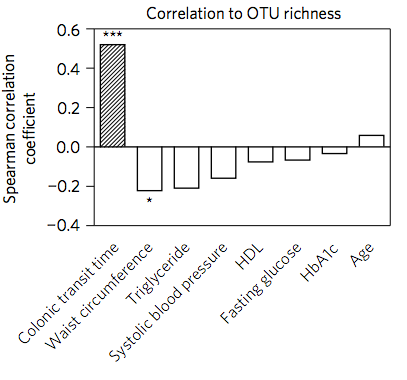
Correlations of colonic transit time with a number of variables - above the line indicates positive correlation. From doi:10.1038/nmicrobiol.2016.93
The time it took for the markers to make their way through the gut was positively correlated with microbial diversity - that is longer transit time meant more diversity.
The authors then looked at the effects on metabolism. Microbes are capable of breaking down a huge number of compounds that we cannot, and the products of this metabolism make their way into our bloodstream. Many of these metabolites were altered in subjects with long transit times, suggesting (again, not surprising) that the more time the things we ingest hang out in the gut, the more that microbes can spend breaking them down.
This isn’t all good news - microbial metabolism isn’t an unalloyed good. Microbes go after sugars first, and often excrete short-chain fatty acids (SCFAs), which positively regulate the immune system, and have been associated with a number of positive effects. But they’ll switch to extracting energy from proteins if the sugars are depleted and some of the waste products from this protein metabolism aren’t great for our health. These detrimental metabolites were elevated in people with very long colonic transit times.
This study is mostly observational, and provides us with another list of correlations, rather than a clear picture of causal relationships. But it’s another reminder that the links between our guts, our microbes and are health are likely far more complicated than we currently imagine.
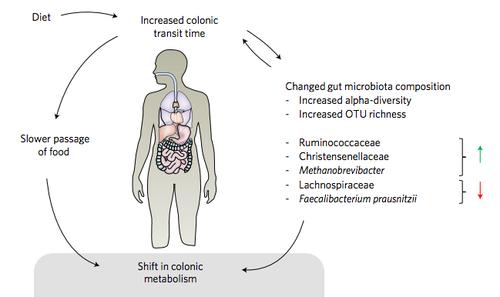
From doi:10.1038/nmicrobiol.2016.93