This article was published in Scientific American’s former blog network and reflects the views of the author, not necessarily those of Scientific American
A few weeks ago, I heard a wonderful interview of the president of the World Bank Jim Yong Kim, and towards the end (around the 1 hour mark), he spent a bunch of time talking about childhood stunting. These physiological effects of poor nutrition are seen in a shockingly large number of children around the world and have profound implications on brain development, learning, and ultimately the economic future of these children.
Unfortunately, when a child is suffering from malnutrition, it can be difficult to intervene to correct the problem. About this time last year, I wrote about research showing that malnutrition significantly and persistently alters the gut microbiome of young children, and that these microbes perpetuated the effects of malnutrition.
In other words, getting undernourished kids more calories is not enough - maybe we need to get them better microbes too.
On supporting science journalism
If you're enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
Then late last month, I read about new research from Jeff Gordon’s lab identifying a potential way to get those better microbes by analyzing the breast milk of mothers with healthy or stunted children.
The logic goes like this: We know that breast milk doesn’t only feed the infant, it also feeds the infant’s bacteria. Since there are identifiable differences in the microbial composition of stunted and healthy baby intestines, maybe there are identifiable differences in the milk of the mothers of these children. Further, maybe those differences will point the way to better interventions for stunted infants to get their microbiota on the right track.
In particular, we know that certain oligosaccharides - chains of sugar molecules - in breast milk are not absorbed by infant intestines, but seem to be in breast milk exclusively to nurture good gut bugs. So Mark Charbonneau and his co-authors chemically examined the oligosaccharide content of the milk from mothers of healthy children and compared them to the milk from mothers of stunted children.
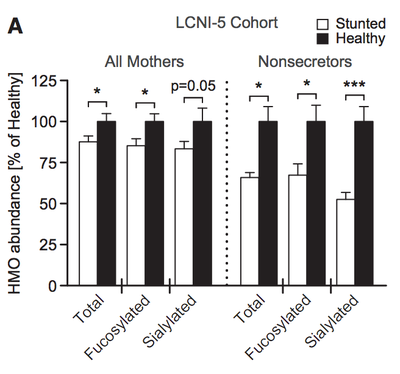
Levels of human milk oligosaccharides (HMS in the mothers of healthy (black bars) or stunted (white bars) children. “Fucosylated” and “Sialylated” are just different kinds of HMOs with slightly different chemical compositions. Figure 1a from doi:10.1016/j.cell.2016.01.024
Consistent with their hypothesis, Charbonneau et. al. found lower levels of these sugars in the milk from the mothers of stunted infants, and these differences were exacerbated in women that did not have a functional FUT2 gene (non-secretors).
But does this difference matter? The authors followed up this observation by replacing the gut microbiome of mice with the microbiome of one of the undernourished kids and fed it a typical regional diet (the cohort was in Malawi) either with or without sialylated milk oligosaccharides from cows (bovines, thus BMOs). Importantly, they made sure the total calories consumed by the mice stayed constant, but the mice that got the BMOs put on more weight than those that didn’t. Mice that also were supplemented with inulin, a similar sugar that’s often found in baby formula (but chemically distinct from HMOs did not put on much extra weight.
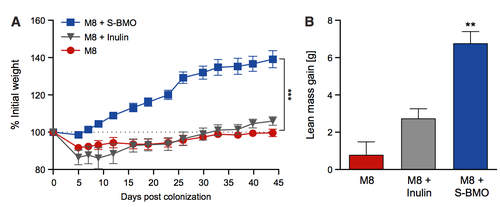
Mice with the microbiota of student human infants were able to grow much better when their diet was supplemented with sialylated milk oligosaccharides, but not with inulin. Figure 2a and 2b from doi:10.1016/j.cell.2016.01.024
The authors also did a bunch of work to characterize the response of the gut microbes to these sugars, and to draw a plausible link between the metabolism of the bacteria and the changes observed in the mouse. There are a lot of caveats with this study - a human microbiome in a mouse gut fed with cow milk sugars - but the data suggest that there’s something important here. More importantly, they suggest a plausible path to intervene in the development of malnourished children. Previous attempts to recover developmental delays have not worked out well. Perhaps we need to feed an undernourished microbiome too.
