This article was published in Scientific American’s former blog network and reflects the views of the author, not necessarily those of Scientific American
The most unexpected beneficiary of the EF-5 tornado that struck Joplin, Missouri, on May 22, 2011 was a fungus named Apophysomyces.
It may, in fact, have been the only beneficiary. The mile-wide tornado touched down just to the west of Joplin that day and rampaged through town. The people of Joplin endured a maelstrom of metal, wood, and rock hurled at over 200 miles per hour. 158 people died and more than 1,100 were injured in this single storm; almost half the town was destroyed.
In the weeks after, doctors started to notice something strange among a few of those injured. Their wounds were blackening, infected by fungi so aggressive that the flesh actually sprouted fuzzy white mold, as if they were a forgotten orange or loaf of bread.
On supporting science journalism
If you're enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
Doctors sampled the wounds, grew the fungus in the lab, and were astonished to find 13 people had all become infected by a single fungus rarely seen in humans: Apophysomyces trapeziformis. Only 74 cases had ever been recorded. This time, the fungus would go on to kill or contribute to the deaths of five of the 13.
Apophysomyces is a zygomycete, one of the five major groups of fungi. Zygomycetes get their name from the special reproductive structure in which they have sex and make sexual spores: the zygosporangium. It looks like a big dark nut created at the junction where two fungal filaments of opposite mating type (i.e. sex) meet.
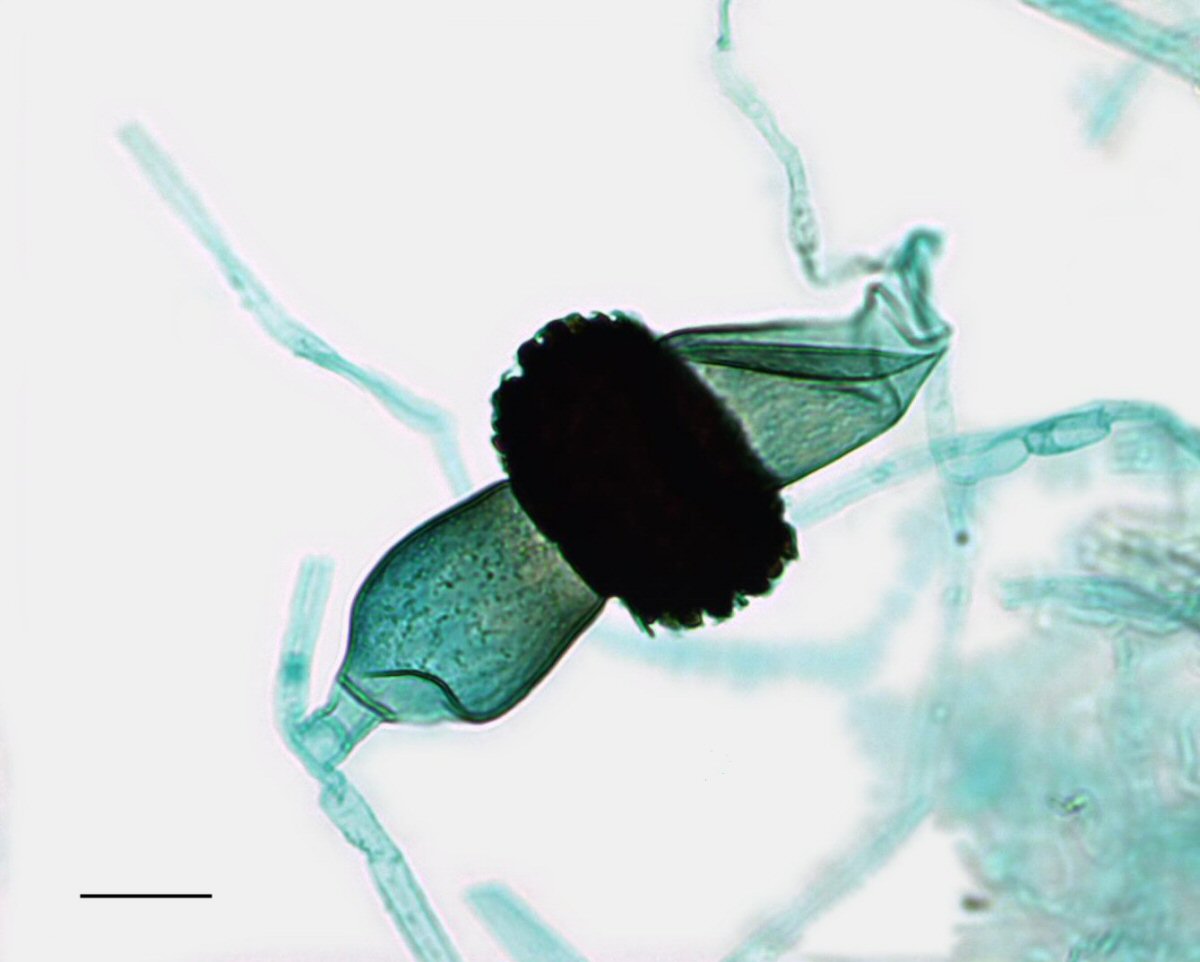
Fungal filaments artificially stained blue here. "Zygo1003" by Jon Houseman - Jon Houseman and Matthew Ford. Licensed under CC BY-SA 3.0 via Wikimedia Commons.
Many zygomycetes are saprobes that make a living eating dead plants. A few parasitize insects or other fungi. Under normal conditions, Apophysomyces scavanges dead plants and can no more infect a human than order a pizza. That rulebook gets tossed out, however, when an object traveling in excess of 200 miles per hour injects the fungus directly into human flesh.
Once comfortably ensconced in the human body, it wastes no time in taking over the place. The torrid conditions don't seem to bother it, nor does the presence of a fully armed and operational immune system. According to Glenn Roberts, a professor of laboratory medicine, pathology, and microbiologiy and a consultant in the division of clinical microbiology at the Mayo Clinic in Rochester, Minnesota, in the laboratory Apophysomyces is referred to as a “lid lifter” because within a matter of hours the fungus can grow from a single spore to a mass of filaments that literally raises the roof of its Petri dish and crawls down the sides.
Matters are no different in the human body. The fungus is particularly good at infiltrating the walls and insides of blood vessels, where its filaments form nets that filter red and white blood cells from blood plasma, creating a clot. The clot blocks blood flow to the tissue, which dies, blackens, and as mentioned earlier, may actually sprout a fuzzy coating of mold.
Warning: The following image is extremely graphic.
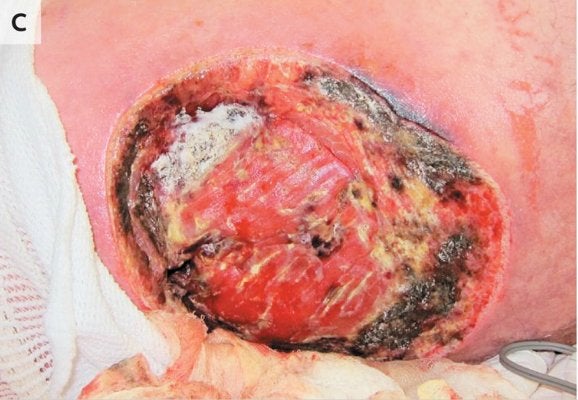
Mold of Apophysomyces growing on the wound of a person injured in the Joplin tornado. Fig. 1c from Neblett Fanfair, et al. 2012. Click here for source.
Doctors treat the infection with antifungal drugs and slice away the dead flesh, a process rather aseptically termed “debridement”. Brutally, those infected in Joplin underwent an average of four debridements. The fungus grew so fast into the tissue and bone of one patient who had suffered a deep wound to his upper chest that doctors had to replace at least part of it with a titanium rib cage.
Of the five patients who died, all did so within two weeks of samples being taken, and all were still infected when they died. For three of the five, the fungus was listed as a primary or contributing cause of death on the death certificate. Unfortunately, no autopsy was performed in any of the deaths – part of a trend that David Dobbs has documented and rightly lamented -- making it difficult to be certain whether the fungus was the cause or not.
Were there any clues to what made people likely to get infected? A team of scientists from the CDC, the Missouri Department of Health and Senior Services, the University of Texas Health Science Center, and the Translational Genomics Research Institute conducted a case-control study in order to find out. They published their results in the New England Journal of Medicine the following year.
Having many puncture wounds or lacerations was most correlated with Apophysomyces infection. And all 13 of those who became infected had also been in the zone of greatest destruction during the storm. Interestingly, none of the patients infected by the fungus in Joplin who were in single-family homes at the time of the tornado (a total of nine) had access to a basement, safe room, or storm shelter.
This is not the first time that Apophysomyces has been turned up after a natural disaster. Two people injured during the 2004 Indian Ocean tsunami were infected by it, as were eight people after a 1985 volcano eruption in Colombia. In nearly all cases, penetrating trauma was the common denominator.
This left the question of the source of the fungus. Genotyping of the fungi isolated from wounds detected that there were three clusters of nearly-identical fungi and a few other less closely related strains of Apophysomyces. All of the fungi, whether in a cluster or not, were more closely related to each other than to control isolates of the fungus. That suggests that several genetically distinct populations of the fungus were involved but that all of them were local, the team said.
However, plotting four of the types on a map of victim locations during the storm did not, unsurprisingly, reveal any patterns. Surely there is no better way of scrambling inoculum sources than the vicious winds of an F-5 tornado.
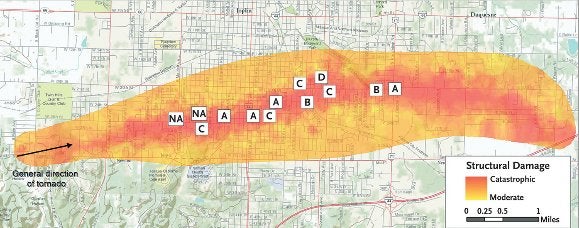
"The letters A through D denote the subtype groups of Apophysomyces trapeziformis clinical isolates from 11 patients; for 2 patients, data on the subtype group were not available (NA). On this map, the locations of case patients at the time of the tornado have been randomly shifted from 0.2 to 0.4 km (0.1 to 0.25 mi) in order to protect patient confidentiality. Data are from the U.S. Army Corps of Engineers and Esri." Fig. 2 from Neblett Fanfair et al. 2012. Click here for source.
The pattern – or lack thereof – suggested to the scientists who studied it one of two scenarios. The tornado may have disturbed a single innoculum source containing a variety of strains of Apophysomyces soon after touchdown on the west side of town. It then spread these spores through the city. Or the tornado disturbed multiple sources along its path, each containing one or more strains.
Interestingly, searches following the tornado were unable to detect the presence of Apophysomyces in the Joplin area. And although two tornadoes touched down in Alabama and Massachusetts around the same time as the Joplin twister, the state health departments reported no Apophysomyces infections in those injured.
In a letter to the editor of the New England Journal of Medicine published three months after the initial article, two military physicians wrote to say they have observed, "increasing rates of trauma-related invasive fungal infections" Furthermore, 50% of the combat troops that had wounds infected by fungi in Afghanistan proved to be zygomycete fungi, and up to one-third of those were co-infected with molds from a different group of fungi as well. Impressively, and perhaps because of the general fitness of soldiers, the mortality rate was only 7.9%. In Joplin, it was potentially 38%.
Three physicians from Children's Mercy Hospital in Kansas City who had treated two of the patients infected with Apophysomyces by the Joplin tornado also wrote a letter to the editor. They agreed that “the extent of injury in our patients was typical of those seen in combat-related wounds”, and urged consultation with experienced combat surgeons in the wake of future tornadoes or other “catastrophic disasters”.
However, they had also stumbled on an ominous finding. In addition to Apophysomyces, the Kansas City physicians identified multidrug-resistant gram-negative bacteria in the patients' wounds. As if an F-5 tornado and flesh-eating fungus were not enough, the scientists surmised that because the tornado struck farmland, agricultural antibiotic use among cattle and other livestock may have played a role in exposing these victims to yet another deadly peril.
Correction 7/29/15: This article initially stated that 50% of all combat soldiers with injuries in Afghanistan were infected by zygomycete fungi. In reality, 50% of all combat soliders with wounds infected by fungi were infected with zygomcyetes. The author apologizes for the error.
References
Etienne, Kizee A., John Gillece, Remy Hilsabeck, Jim M. Schupp, Rebecca Colman, Shawn R. Lockhart, Lalitha Gade et al. "Whole genome sequence typing to investigate the Apophysomyces outbreak following a tornado in Joplin, Missouri, 2011." PloS ONE (2012): e49989.
Neblett Fanfair, Robyn, Kaitlin Benedict, John Bos, Sarah D. Bennett, Yi-Chun Lo, Tolu Adebanjo, Kizee Etienne et al. "Necrotizing cutaneous mucormycosis after a tornado in Joplin, Missouri, in 2011." New England Journal of Medicine 367, no. 23 (2012): 2214-2225.